Diabetes
Diabetes is a chronic (long-lasting) health condition that affects how your body turns food into energy.
Most of the food you eat is broken down by your digestive system into sugar (glucose) and released into your bloodstream. When your blood sugar goes up, your pancreas gets signaled to release insulin. Insulin is a key to let the blood sugar into your body’s cells for use as energy.
If you have diabetes, your body either doesn’t make enough insulin or can’t use the insulin it makes as well as it should. When that happens, too much blood sugar stays in your bloodstream. Over time, that can cause serious health issues, such as heart disease, vision loss, and kidney disease.
There isn’t a cure for diabetes at this time, but losing weight, eating healthy food, and being active can really help manage your condition and improve health. Taking medicine as directed by your doctor, getting diabetes self-management education and support, and keeping health care appointments can also reduce the impact of diabetes on your life.
Types of Diabetes
There are three main types of diabetes: type 1, type 2, and gestational diabetes (diabetes while pregnant).
- Type 1 Diabetes
Type 1 diabetes is due to an autoimmune reaction (the body attacks itself by mistake) that stops your body from making insulin. Approximately 5-10% of the people who have diabetes have type 1. Symptoms of type 1 diabetes can often develop quickly. It’s usually diagnosed in children, teens, and young adults. If you have type 1 diabetes, you’ll need to take insulin every day to survive. Currently, no one knows how to prevent type 1 diabetes.
- Type 2 Diabetes
With type 2 diabetes, your body doesn’t use insulin well and can’t keep blood sugar at normal levels. About 90-95% of people with diabetes have type 2. It develops over many years and is usually diagnosed in adults (but is also found more and more in children, teens, and young adults). You may not notice any symptoms, so it’s important to get your blood sugar tested if you’re at risk. Type 2 diabetes can be prevented or delayed with healthy lifestyle changes, such as losing weight, eating healthy food, and being active.
- Gestational Diabetes
Gestational diabetes develops in pregnant women who have never had diabetes. If you have gestational diabetes, your baby could be at higher risk for health problems. Gestational diabetes usually goes away after your baby is born but increases your risk for type 2 diabetes later in life. Your baby is more likely to have obesity as a child or teen, and more likely to develop type 2 diabetes later in life too.
- Prediabetes
In the United States, 88 million adults—more than 1 in 3—have prediabetes. What’s more, more than 84% of them don’t know they have it. With prediabetes, blood sugar levels are higher than normal, but not high enough yet to be diagnosed as type 2 diabetes. Prediabetes raises your risk for type 2 diabetes, heart disease, and stroke. The good news is if you have prediabetes, a CDC-recognized lifestyle change program can help you take healthy steps to reverse it.
Diabetes by the Numbers
- 37.3 million Americans—about 1 in 10—have diabetes, and 1 in 5 of them don’t know they have it.
- Diabetes is the seventh leading cause of death in the United States.
- Diabetes is the #1 cause of kidney failure, lower-limb amputations, and adult blindness.
- In the last 20 years, the number of adults diagnosed with diabetes has more than doubled.
Diabetes Symptoms
The following symptoms of diabetes are typical. However, some people with type 2 diabetes have symptoms so mild that they go unnoticed.
Common symptoms of diabetes:
- Urinating often
- Feeling very thirsty
- Feeling very hungry—even though you are eating
- Extreme fatigue
- Blurry vision
- Cuts/bruises that are slow to heal
- Weight loss—even though you are eating more
- Tingling, pain, or numbness in the hands/feet
Source: Type 2 Diabetes - Symptoms | ADA
Diabetes Prevention and Management
5 Tips for Taking Control
Lifestyle changes can help prevent the onset of type 2 diabetes, the most common form of the disease. Making a few changes in your lifestyle now may help you avoid the serious health complications of diabetes in the future, such as nerve, kidney and heart damage.
1. Lose extra weight
Losing extra weight reduces the risk of diabetes. People in one large study reduced their risk of developing diabetes by almost 60% after losing approximately 7% of their body weight with changes in exercise and diet.
Set a weight-loss goal based on your current body weight. Talk to your doctor about reasonable short-term goals and expectations, such as a losing 1 to 2 pounds a week.
2. Be more physically active
There are many benefits to regular physical activity. Exercise can help you:
- Lose weight
- Lower your blood sugar
- Boost your sensitivity to insulin
Goals for most adults to promote weight loss and maintain a healthy weight include:
- Aerobic exercise.Aim for 30 minutes of aerobic exercise each day such as brisk walking, swimming or biking for a total of at least 150 minutes a week.
- Resistance exercise.Resistance exercise such as weightlifting or yoga at least 2 to 3 times a week increases your strength, balance and ability to maintain an active life.
- Limited inactivity.Break up long bouts of inactivity, such as sitting at the computer, can help control blood sugar levels. Take a few minutes to stand, walk around or do some light activity every 30 minutes.
3. Eat healthy plant foods
Plants provide vitamins, minerals and carbohydrates in your diet. Fiber-rich foods promote weight loss and lower the risk of diabetes. Eat a variety of healthy, fiber-rich foods, which include:
- Fruits
- Nonstarchy vegetables, such as leafy greens, broccoli and cauliflower
- Legumes, such as beans and chickpeas
- Whole grains, such as whole-wheat pasta and bread.
The benefits of fiber include:
- Slowing the absorption of sugars and lowering blood sugar levels
- Interfering with the absorption of fat and cholesterol
- Managing other risk factors such as blood pressure and inflammation
- Helping you eat less because fiber-rich foods are more filling and energy rich
Avoid foods that are "bad carbohydrates" — high in sugar with little fiber or nutrients: white bread and pastries, pasta from white flour, fruit juices, and processed foods with sugar or high-fructose corn syrup.
4. Eat healthy fats
Fatty foods are high in calories and should be eaten in moderation. To help lose and manage weight, your diet should include a variety of foods with unsaturated fats, sometimes called "good fats."
Sources of good fats include:
- Olive, sunflower, and canola oils
- Nuts and seeds, such as almonds and peanuts
- Fatty fish, such as salmon and tuna
Saturated fats, the "bad fats," are found in dairy products and meats. These should be a small part of your diet. You can limit saturated fats by eating low-fat dairy products and lean chicken and pork.
5. Skip fad diets and make healthier choices
Many fad diets — such as the glycemic index, paleo or keto diets — may help you lose weight. There is little research, however, about the long-term benefits of these diets or their benefit in preventing diabetes.
Your dietary goal should be to lose weight and then maintain a healthier weight. Healthy dietary decisions need to include a strategy that you can maintain as a lifelong habit.
One simple strategy to help you make good food choices and eat appropriate portions sizes is to divide up your plate. These three divisions on your plate promote healthy eating:
- One-half: fruit and nonstarchy vegetables
- One-quarter: whole grains
- One-quarter: protein-rich foods, such as legumes, fish or lean meats
When to see your doctor
The American Diabetes Association recommends routine screening with diagnostic tests for type 2 diabetes for all adults age 45 or older and for the following groups:
- People younger than 45 who are overweight or obese and have one or more risk factors associated with diabetes
- Women who have had gestational diabetes
- People who have been diagnosed with prediabetes
- Children who are overweight or obese and who have a family history of type 2 diabetes or other risk factors
If you have diabetes, the following are goals that you and you’re your doctor will work together to achieve:
Diabetes Management Goals (as per National Committee for Quality Assurance guidelines):
- Maintaining a HgbA1C level under 7%
- Maintaining good blood pressure control under 140/90
- Maintaining good cholesterol level control (LDL≤100)
- Routine monitoring for diabetic kidney disease (nephropathy)
- Routine monitoring for diabetic eye disease (retinopathy)
Diabetes Screenings
Eye Screening for People with Diabetes
Optometrists and ophthalmologists are eye care specialists who play an important role in the early detection and timely treatment of diabetes-related eye diseases such as retinopathy, glaucoma, and cataracts.
These conditions can be avoided or delayed with annual dilated eye examinations.
Although people with diabetes are at a higher risk of vision loss and eye diseases, 60% do not get annual eye exams.
In the United States:
- People with diabetes have a 25 times higher risk of blindness than those without
- Diabetic retinopathy is the leading cause of blindness. Glaucoma, cataracts, and other eye disorders occur earlier and more often in people with diabetes.
- More than 90% of vision loss caused by diabetes can be avoided with early detection and treatment.
See an eye care professional every year, and as soon as possible if you have the following symptoms:
- Dark, floating spots or streaks.
- Dry eyes.
- Changes in the ability to see clearly, focus, or adjust to changes in light or darkness that are sudden
- Double vision or difficulty focusing due to vision fluctuations
Source: https://www.cdc.gov/diabetes/professional-info/health-care-pro/diabetes-eye-health.html
HbA1c Screening
Get an A1C test to find out your average blood sugar levels. It is very important to know if you’re at risk for prediabetes or type 2 diabetes, or if you have been diagnosed as having type 2 diabetes, to know that your condition is well managed.
The A1C test, which is also known as the hemoglobin A1C or HbA1c test, is a simple blood test that measures your average blood sugar levels over the past 3 months. It’s one of the commonly used tests to diagnose prediabetes and diabetes, and is also used to help you and your health care team manage your diabetes. Higher A1C levels can lead to diabetes complications, so reaching and maintaining your A1C goal of less than 7% is imperative if you have diabetes.
What Does the A1C Test Measure?
When sugar enters your bloodstream, it attaches to hemoglobin, a protein in your red blood cells. The A1C test measures the percentage of your red blood cells that have sugar-coated hemoglobin.
Who Should Get an A1C Test, and When?
Testing for diabetes or prediabetes:
All adults over 45 should get a baseline A1C, as well as those under 45 who are overweight and have one or more risk factors for prediabetes or type 2 diabetes:
- If you are over 45 and your test results come back normal, but you have risk factors or have had gestational diabetes, you should retest every 3 years.
- If your result shows you have prediabetes, talk to your doctor about what steps to take to improve your health and lower your risk to develop type 2 diabetes. Retest as recommended by your doctor, usually every 1 to 2 years.
- If you are symptom free but your result shows you have prediabetes or diabetes, test for a second time to confirm results.
- If your test shows you have diabetes, talk to your doctor about diabetes management plan to keep you healthy. You may wish to speak to a dietician about changing your diet to keep your blood sugar at appropriate levels.
Managing diabetes:
If you have diabetes, get an A1C test at a minimum twice a year, more often if your medicine changes or if you have other health conditions. Your doctor would know best how often is right for you.
How to Prepare for Your A1C Test:
The test is done in a doctor’s office or a lab using a sample of blood from a finger stick or from your arm. Nothing special is needed to be done to prepare for your A1C test.
Your A1C Result
Diagnosing Prediabetes or Diabetes
| Normal | Below 5.7% |
| Prediabetes | 5.7% to 6.4% |
| Diabetes | 6.5% or above |
A normal A1C level is below 5.7%, a reading of 5.7% to 6.4% indicates prediabetes, and a level of 6.5% or more indicates diabetes. In the prediabetic range, the higher your A1C, the greater risk you have to develop type 2 diabetes.
Managing Diabetes
Your A1C result can also be reported as estimated average glucose (eAG), the same numbers (mg/dL) you would see on your blood sugar meter:
|
A1C % |
eAG mg/dL |
|
7 |
154 |
|
8 |
183 |
|
9 |
212 |
|
10 |
240 |
What Can Affect Your A1C Result?
Get your A1C tested in addition to regular blood sugar self-testing if you have diabetes.
Several factors can give a false increase or decrease to your A1C result, including:
- Kidney failure, liver disease, or severe anemia.
- A less common type of hemoglobin that people of African, Mediterranean, or Southeast Asian descent and people with certain blood disorders (such as sickle cell anemia or thalassemia) may have.
- Certain medicines, including opioids and some HIV medications.
- Blood loss or blood transfusions.
- Early or late pregnancy.
If any of these factors apply to you, speak to your doctor to see if additional testing is needed.
Your A1C Goal
The goal for most people with diabetes is 7% or below. However, there are many factors that can affect your personal goal including your age and other medical conditions. You and your doctor together should set your own individual A1C goal.
Younger people that will live with diabetes for many years may have a lower A1C goal so as to reduce the risk of complications, unless they often have hypoglycemia (low blood sugar). Older people that have severe lows, or have other serious health complications may have a higher A1C goal.
Remember, A1C is one of the important tools for managing diabetes, it doesn’t replace blood sugar testing at home. Blood sugar fluctuates throughout the day and night, which isn’t shown by your A1C. Two people can have the exact same A1C, but one can have steady blood sugar and one can swing between highs and lows.
If you’re reaching your A1C goal but having the high and low swings, check your blood sugar more often and at different times throughout the day. Keep track and share the results with your doctor.
Source: https://www.cdc.gov/diabetes/managing/managing-blood-sugar/a1c.html
Chronic Kidney Disease Screening for people with diabetes
If you have diabetes, ask your doctor about kidney disease.
Chronic kidney disease (CKD) often develops slowly and with few symptoms. Many people don’t realize they have CKD until it’s advanced and they need dialysis (a treatment that filters the blood) or a kidney transplant to survive.
If you have diabetes, get your kidneys checked regularly, which is done by your doctor with simple blood and urine tests. Regular testing is your best chance for identifying CKD early if you do develop it. Early treatment is most effective and can help prevent additional health problems.
CKD is common in people with diabetes. Approximately 1 in 3 adults with diabetes has CKD. Both type 1 and type 2 diabetes can cause kidney disease.
Source: https://www.cdc.gov/kidneydisease/prevention-risk.html
Find a Provider
Diabetes is typically managed by a primary care physician. Choose your MagnaCare health plan; then search for Primary Care Physician in the Find a Provider menu.
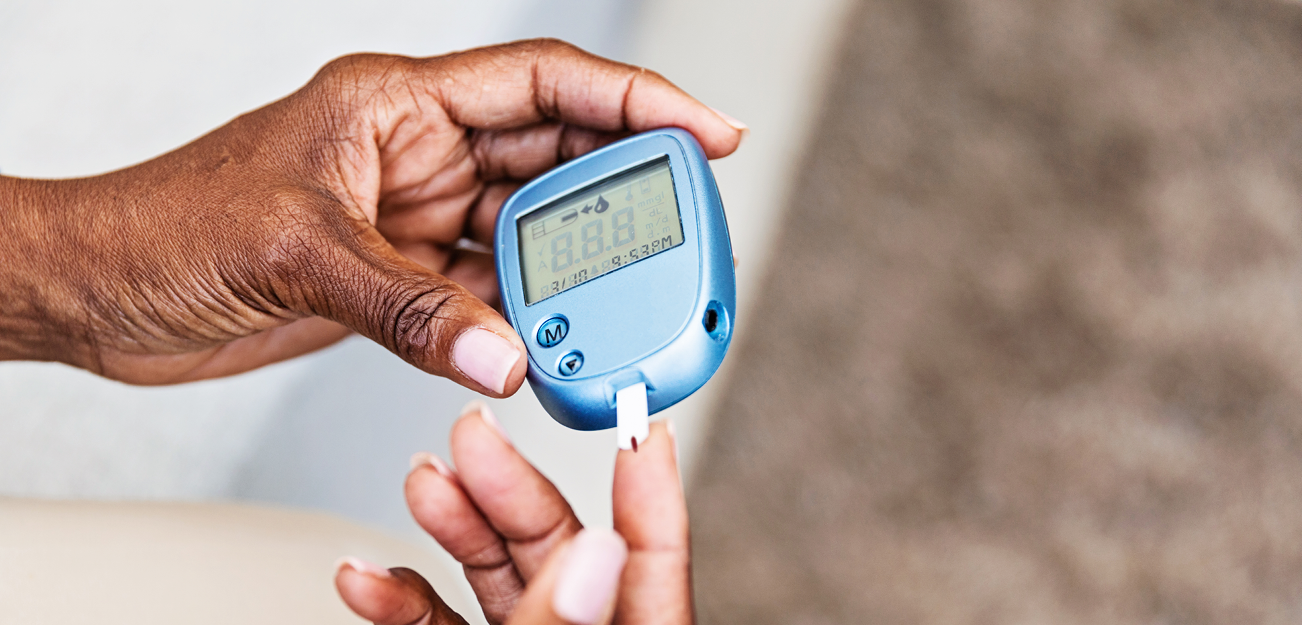

Diabetes HbA1c Screening
Get an A1C test to find out your average blood sugar levels. It is very important to know if you’re at risk for prediabetes or type 2 diabetes, or if you have been diagnosed as having type 2 diabetes, to know that your condition is well managed. The A1C test, which is...

The country's leading diabetes organization, it's mission is to prevent and cure diabetes and to improve the lives of all people affected by diabetes. Learn More >

The CDC is the leading national institute of public health. It is part of the US Department of Health and Human Services. The CDC provides a wealth of guidance on living with diabetes. Learn More >
